Archive for April, 2011
Safe Travels on Your Infertility Journey
 By Dr. Craig R. Sweet, Medical Director & Founder
By Dr. Craig R. Sweet, Medical Director & Founder
I sit here wondering what I can write about that others will not already be commenting on during this very busy and important National Infertility Awareness Week for those traveling the infertility journey. But after over 20 years of taking care of tens of thousands of patients, I have developed a few philosophical perspectives and “rules of the road” and I want to share with you.
Don’t Wait Until All Your Ducks Are in a Row
First, a woman’s ability to conquer the world does not necessarily transfer to conquering the biologic clock that endlessly ticks forward. My IVF patients already are arriving at my doorstep at an average age of close to 37, which puts them at a significant disadvantage. If I could encourage young women to do anything, it would be to try to start their families earlier. If they wait to have all their “ducks in a row,” they may never see their little ducklings.
Hollywood is rife with women conceiving late in life, but they rarely tell anyone that they used donated eggs, not that it is our business. Please, I implore women around the world to have their children sooner and not depend on our modestly advanced technologies to prevail when nature argues differently.
Seek Knowledge Sooner Rather Than Later
Second, if you are having problems conceiving, see a knowledgeable local reproductive endocrinologist sooner rather than later. Don’t be  pressured to start a more intensive evaluation or procedures one day earlier than you are ready but seek knowledge sooner. Obtain an opinion from someone you trust to see where you stand and to get a glimpse into your reproductive future. At the risk if alienating some referring physicians, do not be satisfied with seeing general OB/GYN physicians or Urologists to seek solid information should problems be found. Knowledge is power; obtain it quickly with experts who live and breath your issues each and every day.
pressured to start a more intensive evaluation or procedures one day earlier than you are ready but seek knowledge sooner. Obtain an opinion from someone you trust to see where you stand and to get a glimpse into your reproductive future. At the risk if alienating some referring physicians, do not be satisfied with seeing general OB/GYN physicians or Urologists to seek solid information should problems be found. Knowledge is power; obtain it quickly with experts who live and breath your issues each and every day.
Don’t Be Afraid of the Unknown
Third, don’t be afraid of what you might find. Take a deep breath and learn the truth. I see far too many patients that fear for too long, only to find out their fears were incorrect, or that their delay significantly impaired their overall chances for success while inadvertently increasing their costs to succeed. Be brave, find support and gain knowledge quickly. Do not be afraid. This is absolutely directed at both the male and female patients.
In Closing
I will leave it up to RESOLVE and many other organizations to do what they do best: organizing patients to speak with one united voice during this very important week. During this week of attention, a philosophical perspective may really be of some benefit hopefully heard among the din of all the other conversations.
Infertility is a journey and what journey should start without a few rules of the road?
Craig R. Sweet, M.D.
Founder, Embryo Donation International
Reproductive Endocrinologist
Medical & Laboratory Director
The Disposition of Cryopreserved Embryos
 By Dr. Craig R. Sweet, Medical Director & Founder
By Dr. Craig R. Sweet, Medical Director & Founder
During in vitro fertilization (IVF), numerous eggs are removed from the woman, and fertilized with sperm to create embryos that are grown in the laboratory for several days. Almost always the final number of embryos available for transfer is less than the number of eggs (oocytes) originally retrieved from the woman.
For example:
- 12-14 oocytes retrieved
- 10-12 mature ooctyes (available for fertilization)
- 8-10 oocytes successfully fertilize with sperm
- 3-6 embryos survive and are available for transfer or storage in liquid nitrogen for future use
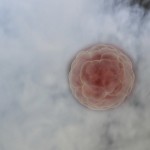
From the few embryos left on day five of fertilization, we try to transfer the smallest number needed to achieve a pregnancy. Approximately, one-third of the patients will have enough extra embryos to freeze for future use.
These embryos may last for decades frozen in liquid nitrogen (Mazur P, 1980). For many, deciding what to do with the embryos is a very difficult decision. In general, the following options exist:
- Thaw and transfer for personal use
- Donate to science
- — Human embryonic stem cell research
- — Other valuable studies
- Discard
- — Thaw and dispose
- — “Compassionate Transfer” into a uterus at a time when implantation cannot occur
- Donate to patients in need (i.e., embryo donation)
Many, but not all facilities, offer the “discard” option. We believe that better choices exist than destruction and no longer include it in our patient consents. The actual options available to a given patient may be more limited than the list above.
There are many reasons patients do not use the embryos for personal use (Kirkman M, 2003):
- They have completed their family
- Past pregnancy complications
- Age
- Emotional exhaustion
- Cannot afford further treatment
- Divorced
Many find deciding the next steps for their cryopreserved embryos to be exquisitely difficult. I feel that all reproductive facilities could perform far better at counseling patients and assisting them in making these decisions. Patients have complained that we haven’t done an adequate job (Nachtigall RD, et al., 2005). I suspect they are right. I believe it is the responsibility of the cryopreservation or reproductive endocrine facility to educate patients adequately and offer assistance and information when requested. EDI designed a brief brochure to address these very issues.
If one is really uncertain and the personal use of the embryos is still a possibility, then I agree that the embryos should be stored longer, but not indefinitely.  If, however, additional family building has been ruled out, then I advise the patient to take a deep breath and make the difficult decision that ultimately must be made.
If, however, additional family building has been ruled out, then I advise the patient to take a deep breath and make the difficult decision that ultimately must be made.
My patients put so much, emotionally and financially, into the creation of their embryos. Our goal is to support them through the difficult decision, no matter what they decide. I can only hope they will consider either human embryonic stem cell research or embryo donation. I personally believe embryos deserve a heightened level of respect. These two possible destinations serve a common and greater good for everyone involved. While human embryonic stem cell research holds some future promise, the immediacy of growing a family though embryo donation seems to be the best choice for those wonderful and precious gifts, a donors’ embryos.
Craig R. Sweet, M.D.
Founder, Embryo Donation International
Reproductive Endocrinologist
Medical & Laboratory Director
References:
- Kirkman M. Egg and Embryo Donation and the Meaning of Motherhood. Women & Health 2003;38(2):1-18.
- Mazur P. Limits to life at low temperatures and at reduce water contents and water activities. Orig Life 1980:10(2):137-59.
- Nachtigall RD,et al. Parents’ conceptualization of their frozen embryos complicates the disposition decision. Fertil Steril 2005;84:431-4.
Welcome to Embryo Donation International
Hello and welcome to the Embryo Donation International blog! We will be discussing all things related to embryo donation – the process, guidelines, regulations and the tough decisions that go into the final decision.
Who is Embryo Donation International (EDI)?
Embryo Donation International (EDI) is a subdivision of Specialists In Reproductive Medicine & Surgery, P.A., which has been providing embryo donation for 10 years making us one of the most experienced embryo donation facilities in the country.
Our mission is to reduce the number of cryopreserved embryos abandoned or discarded by assisting in the matching embryos to patients in need regardless of race, religion, ancestry, sexual preference or marital status. We turned this philosophy into Embryo Donation International.
I started creating our embryo donation program in 2000 and had our first delivery in 2001. I have always enjoyed the field of reproductive ethics, which helped to form many of my philosophies regarding embryo donation. In speaking out against embryo abandonment and the discarding of embryos while speaking out in favor of human embryonic stem cell research, my reproductive endocrine practice began to form the core values we now hold so dearly here at EDI.
At EDI, we believe that the embryos deserve a heightened level of respect; placing them between common cells and the patients we treat. We feel this is a type of gentle embryo advocacy. We believe that they should be used for a common good and have the opportunity to build a family.
For more information, please view the About Us section of the blog or visit our website www.EmbryoDonation.com.
What sets EDI Apart from other Embryo Donation Organizations?
EDI is non-discriminatory. We welcome healthy recipients including single women, homosexual couples, cancer survivors and people of any race or ethnicity. While we believe all healthy embryos deserve a chance at life and that healthy individual deserves a chance at parenthood, we are not a faith-based facility.
We are dedicated to making the process of embryo donation affordable. Our fees are roughly 50-60% less than many alternatives. We also accept embryos from around the world.
Additionally, we have a growing database of embryos (which is available for reviewing at no cost) and we offer them through a variety of means – approved, anonymous and open embryo donation procedures– based on the donors’ wishes and the recipients’ willingness to participate.
We look forward to offering tools for donating or receiving, or simply helping you learn more about the options available along your infertility journey, which we all hope will end with parenthood.
Craig R. Sweet, M.D.
Founder, Embryo Donation International
Reproductive Endocrinologist
Medical & Laboratory Director